Healthcare Payer Solution Market Trends and Insights: Global Forecast to 2030
Uncover key drivers, emerging technologies, and competitive movements shaping the healthcare payer solution market from 2026–2035 with trusted insights from The Business Research Company
What growth pattern is forecast for the Healthcare Payer Solution Market size between 2026 and 2035?
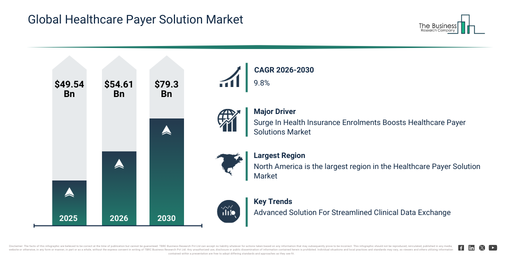
The healthcare payer solution market has seen considerable growth recently. It is forecast to expand from $49.54 billion in 2025 to $54.61 billion in 2026, demonstrating a compound annual growth rate (CAGR) of 10.2%. Historically, this expansion has been propelled by factors such as the increasing complexity of healthcare administration, higher penetration of insurance coverage, the escalating need for claims volume processing, the broadening role of third-party administrators, and the adoption of digital health records.
The healthcare payer solution market is anticipated to experience robust expansion in the coming years, with projections indicating it will reach $79.3 billion by 2030, achieving a compound annual growth rate (CAGR) of 9.8%. This growth during the forecast period can be attributed to several factors, including an increasing shift toward value-based care models, rising investments in cloud-based payer platforms, a growing demand for cost optimization solutions, the expansion of AI-enabled payer analytics, and increasing regulatory reporting requirements. Additionally, major trends expected in the forecast period encompass the increasing adoption of integrated claims management platforms, a rising use of predictive analytics for fraud detection, a growing focus on member-centric engagement solutions, the expansion of automated payment and billing systems, and an enhanced emphasis on regulatory compliance tools.
Access Your Free Sample Report for In-Depth Market Insights:
https://www.thebusinessresearchcompany.com/sample.aspx?id=9393&type=smp
Which Drivers Are Impacting Market Performance In The Healthcare Payer Solution Market?
The anticipated expansion of the healthcare payer solutions market is intrinsically linked to a rise in insurance enrolments. Insurance enrolment refers to the process where a qualified individual registers with an insurance provider to become a member of a plan. Within the insurance market, healthcare payer solutions deliver robust enterprise core administration and claims management platform solutions. These capabilities are crucial for enabling and inspiring expansion, innovation, and cost savings for payer organizations operating across diverse business lines. For instance, in January 2025, reports from the Centers for Medicare & Medicaid Services, a US-based Department of Health and Human Services that provides health coverage through Medicare and Medicaid, indicated that 24.2 million consumers selected plan year 2025 coverage via the Marketplaces during the 2025 Marketplace Open Enrollment Period, including 3.9 million new consumers. This clearly demonstrates how the increasing number of insurance enrolments is driving the demand for the healthcare payer solutions market.
Which Segments Are Contributing To The Growth Of The Healthcare Payer Solution Market?
The healthcare payer solution market covered in this report is segmented –
1) By Services: Business Process Outsourcing Services, Information Technology Outsourcing Services, Knowledge Process Outsourcing Services
2) By Application: Pharmacy Audit And Analysis Systems, Claims Management Services, Fraud Management Services, Computer-assisted Coding (CAC) Systems, Member Eligibility Management Services, Provider Network Management Services, Payment Management Services, Customer Relationship Management Services, Medical Document Management Services
3) By End User: Private Provider, Public Provider
Subsegments:
1) By Business Process Outsourcing Services: Claims Processing, Enrollment And Eligibility Verification, Member Services And Support, Provider Network Management, Billing And Payment Processing, Data Management And Analytics
2) By Information Technology Outsourcing Services: Application Development And Maintenance, IT Infrastructure Management, Data Security And Compliance Solutions, Cloud Services, Software As A Service (SaaS) Solutions
3) By Knowledge Process Outsourcing Services: Clinical Data Management, Healthcare Analytics, Market Research And Intelligence, Medical Coding And Billing Services, Regulatory Compliance Services, Health Outcomes Research
What Upcoming Trends Are Likely To Define The Future Path Of The Healthcare Payer Solution Market?
Leading firms within the healthcare payer solution sector are concentrating on creating sophisticated tools, like Payer Exchange, to manage the increasing quantity of medical records and clinical information. Payer Exchange represents a technological offering engineered to streamline the sharing of clinical data between healthcare service providers and insurers. As an illustration, in June 2023, MRO Corp, a US-based company specializing in clinical data exchange and also in specification-grade architectural lighting, unveiled its Payer Exchange solution. This technology digitizes and automates the process of requesting and fulfilling patient information, thereby decreasing manual tasks for hospital personnel and enhancing operational efficiency. Payer Exchange is designed to address the increasing need from payers for precise and current clinical data, providing a secure, digital link for streamlined communication between providers and payers. The solution prioritizes patient confidentiality, the integrity of data, and the precision of risk adjustment premiums.
Who Are The Prominent Global Companies Shaping The Healthcare Payer Solution Market Landscape?
Major companies operating in the healthcare payer solution market are Cognizant Technical Solutions, Concentrix Corporation, Accenture plc, HCL Technologies Ltd., Xerox Corporation, UnitedHealth Group Inc., McKesson Corporation, HMS Holdings Corp., International Business Machines Corporation, Change Healthcare Inc., Wipro Limited, Infosys Limited, Tata Consultancy Services Limited, NTT Data Corporation, Genpact Limited, Mphasis Limited, Firstsource Solutions Limited, WNS Limited, IQVIA Inc., Omega Healthcare, R1 RCM Inc., Conduent Inc., EXL Service Holdings Inc., Cotiviti Holdings Inc.
Access The Complete Report For Deeper Market Insights:
https://www.thebusinessresearchcompany.com/report/healthcare-payer-solution-global-market-report
Which Region Is Projected To Lead The Healthcare Payer Solution Market During The Forecast Period?
North America was the largest region in the healthcare payer solution market in 2025. The regions covered in the healthcare payer solution market report are Asia-Pacific, South East Asia, Western Europe, Eastern Europe, North America, South America, Middle East, Africa.
Request Your Customized Healthcare Payer Solution Market Research Report for Competitive Advantage:
https://www.thebusinessresearchcompany.com/customise?id=9393&type=smp
Browse Through More Reports Similar to the Global Healthcare Payer Solution Market 2026, By The Business Research Company
Payer Services Market Report 2026
https://www.thebusinessresearchcompany.com/report/payer-services-global-market-report
Healthcare Finance Solutions Market Report 2026
https://www.thebusinessresearchcompany.com/report/healthcare-finance-solutions-global-market-report
Healthcare Reimbursement Market Report 2026
https://www.thebusinessresearchcompany.com/report/healthcare-reimbursement-global-market-report
Get in touch with us:
The Business Research Company: https://www.thebusinessresearchcompany.com/
Americas +1 310-496-7795
Asia +44 7882 955267 & +91 8897263534
Europe +44 7882 955267
Email us at info@tbrc.info
Follow us on:
LinkedIn: https://in.linkedin.com/company/the-business-research-company
YouTube: https://www.youtube.com/channel/UC24_fI0rV8cR5DxlCpgmyFQ
Global Market Model: https://www.thebusinessresearchcompany.com/global-market-model